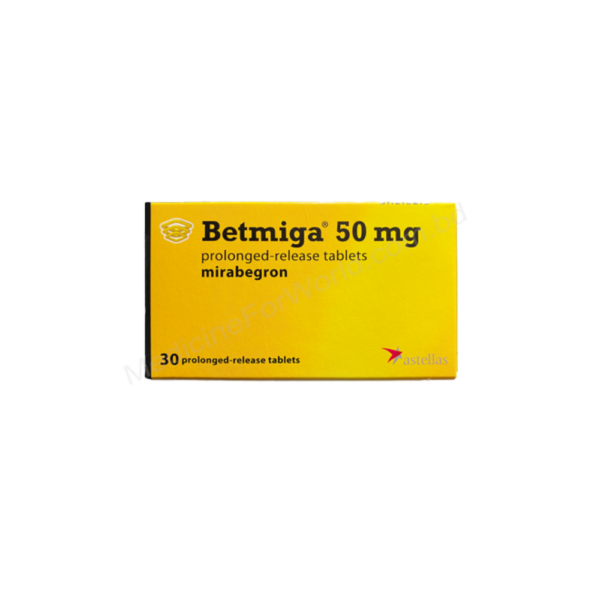
Start Your Incontinence Consultation
Complete a quick and easy questionnaire and one of our prescribers will make sure this treatment is right for you.
4.6/5 Trustpilot Rating

Trusted UK Registered Pharmacy

Takes Under 2 Minutes

Secure and Confidential

Justin Dicks
Superintendent Pharmacist
GPhC Number 2038305
Treatments



Related Medication
Frequently Asked Questions
Have a question? We're here to help
What is urinary incontinence?
Urinary incontinence is the unintentional leakage of urine caused by a loss of bladder control. It can range from occasional small leaks when coughing or sneezing to a strong, sudden urge to urinate that’s difficult to manage. This condition is common, especially among women and older adults, and can often be managed effectively with the right treatment.
What are the different types of urinary incontinence?
The main types are stress incontinence, urge incontinence, and mixed incontinence. Stress incontinence happens when pressure on the bladder (like from coughing or exercise) causes leaks, while urge incontinence involves a sudden, intense need to urinate. Mixed incontinence is a combination of both and understanding which type you have helps guide treatment.
What causes urinary incontinence?
Urinary incontinence can be caused by weakened pelvic floor muscles, bladder muscle overactivity, or nerve issues affecting bladder control. It can also result from pregnancy, menopause, certain medications, or conditions like diabetes. Identifying the underlying cause is important to choose the most effective treatment.
What triggers urinary incontinence?
The common triggers include caffeine, alcohol, and carbonated drinks, as they can irritate the bladder. Sudden movements, laughing, or coughing may also cause leaks in people with stress incontinence. Keeping a bladder diary and avoiding known triggers can help reduce symptoms over time.
What are the symptoms of urinary incontinence?
Symptoms include frequent or urgent urination, accidental leaks, and difficulty holding in urine during everyday activities. Some people may also experience waking up multiple times at night to urinate. The severity varies, but even mild symptoms can impact confidence and quality of life.
How is urinary incontinence treated?
Treatment depends on the type and cause but may include bladder training, pelvic floor exercises, or medication. Prescription treatments like Oxybutynin, Solifenacin or Tolterodine work by relaxing the bladder muscles to reduce urgency and leakage. In more severe cases, medical procedures or lifestyle changes may be recommended by your doctor.
How do urinary incontinence treatments work?
Most medications for incontinence help by calming overactive bladder muscles and improving bladder capacity. This means fewer sudden urges and less frequent trips to the toilet. Regular use as prescribed can greatly improve bladder control and comfort.
How long does urinary incontinence treatment take to work?
It can take a few weeks for medication such as Solifenacin or Tolterodine to show noticeable improvement. Lifestyle changes like pelvic floor exercises may take longer but often provide lasting results. Consistency is key – following your treatment plan daily gives the best chance of success.
Are urinary incontinence treatments safe?
The treatments prescribed for incontinence are generally safe and well-studied. However, some people may experience mild side effects such as dry mouth, constipation, or blurred vision. Always discuss any new symptoms with your doctor or pharmacist, as dose adjustments or alternative medications may help.
Who can use urinary incontinence medication?
Incontinence medication is suitable for most adults experiencing bladder control issues, but not everyone. Those with certain medical conditions such as glaucoma or severe liver problems may need alternative options. It’s important to complete an online consultation or speak to a healthcare professional before starting treatment.
Can urinary incontinence go away on its own?
Mild cases, especially after childbirth or temporary stress, can sometimes improve naturally with time and exercises. However, ongoing or worsening symptoms usually require medical attention. Early treatment helps prevent long-term discomfort and restores confidence in daily life.
What happens if urinary incontinence is left untreated?
If untreated, urinary incontinence can worsen over time and lead to skin irritation, infections, or emotional distress. It can also affect sleep and daily activities, reducing overall quality of life. Seeking help early can make management much easier and more effective.
When should you worry about urinary incontinence?
You should contact a doctor if you experience sudden changes in bladder control, pain while urinating, or blood in your urine. These may indicate a more serious underlying issue. Persistent leakage, even if mild, also deserves attention as effective treatments are available.
Can you drink alcohol when treating urinary incontinence?
Alcohol can irritate the bladder and make symptoms worse by increasing urine production. While small amounts may be tolerated, it’s best to limit alcohol and caffeine when managing incontinence. Staying hydrated with water and avoiding bladder irritants can help treatments work better.
What lifestyle changes help with urinary incontinence?
Strengthening your pelvic floor muscles, maintaining a healthy weight, and avoiding bladder irritants like caffeine can all reduce leaks. Scheduling regular toilet breaks and practising bladder training can also help. Combining these changes with medication gives the best overall results.